— Procedures
Electrophysiology Studies
An Electrophysiology Study is a test of the electrical activity inside your heart to determine where an arrhythmia (abnormal heartbeat) is coming from.
Electrophysiology Studies Explained
An Electrophysiology Study is a test of the electrical activity inside your heart to determine where an arrhythmia (abnormal heartbeat) is coming from.
- What is an Electrophysiology Study?
- What is happening in a heart with arrhythmia?
- Why would I need to have an Electrophysiology Study?
- What happens if you find an abnormality?
- What happens during the procedure?
- Will I feel anything during the procedure?
- How do I prepare for the procedure?
- What happens next?
What is an Electrophysiology Study?
An Electrophysiology Study (EPS) is a test that allows us to take a detailed look at the electrical impulses and pathways inside your heart. By carrying out an EPS, we can work out whether these impulses are causing your heart to beat abnormally (an arrhythmia), and where in the heart those abnormalities are originating.
What is happening in a heart with arrhythmia?
There are four separate chambers in your heart: two upper “atria” and two lower “ventricles”. Your heart can generate electrical charges inside these chambers, prompting them to contract and pump blood around your body. A healthy heart usually beats around 60 to 100 times per minute, at a regular and even pace. The timing of these beats is controlled by the “sinus node”, a patch of cells in one of your atria. Certain medical conditions or events (such as heart attacks and high blood pressure) can produce scarring in the heart tissue, which can disrupt the electrical impulses and cause the natural pacemakers to malfunction. You can read more about arrhythmia in our Heart Rhythm Problems section.
Why would I need to have an Electrophysiology Study?
There are a number of reasons why we might recommend you for an EPS. These include:
- diagnosis: if we suspect you have a heart rhythm problem, or you’re experiencing common arrhythmia symptoms (such as palpitation or fainting), and we want to see what’s going on
- finding out precisely where in your heart the arrhythmia is coming from
- determining whether we can use a procedure called ablation to treat the abnormal impulses
- seeing whether you would benefit from a device to restore natural rhythm to your heart, such as a pacemaker or an internal defibrillator (ICD)
- understanding whether a known heart condition puts you at risk of developing a serious heart problem, such as sudden cardiac death
We may also ask you to do an electrocardiogram test (ECG) alongside your Electrophysiology Study. An ECG also measures electrical impulses, but in less detail than an EPS.
What happens if you find an abnormality?
Once we’ve confirmed an arrhythmia and located its source, we can work out how urgently you need to be treated. Rhythm problems that are coming from the atria are not usually life-threatening, but can be more serious if they originate in the ventricles. In either case, the EPS will help us to put together a comprehensive treatment plan for you. This could be a course of medication or a surgical procedure to target the specific area of cells that is causing the problem (an ablation, which is sometimes performed during the same EPS procedure). Or we may recommend that you have a special monitoring device fitted in your chest, such as a loop recorder, pacemaker or an ICD.
What happens during the procedure?
Electrophysiology Studies work by inserting one or more catheters (fine tubes) into one of your veins, usually in the groin or chest areas; this tube is gently directed through your vein so it runs up to your heart. We then introduce some tiny wires into the tube, possibly using an x-ray device (fluoroscopy) to guide them into position. Once in place, small electrical impulses are passed down the wires to specific areas of your heart. These impulses allow us to detect and record the natural electrical activity that’s happening in your heart (this is known as “cardiac mapping”). We can also stimulate extra beats in your heart in order to detect where the abnormal rhythm is coming from. (We can restore your heart’s natural rhythm using the same procedure.) In some cases we can introduce certain medicines into the catheter to slow or speed up your heart as part of the test. Electrophysiology Studies generally take between one and two hours to complete.
Will I feel anything during the procedure?
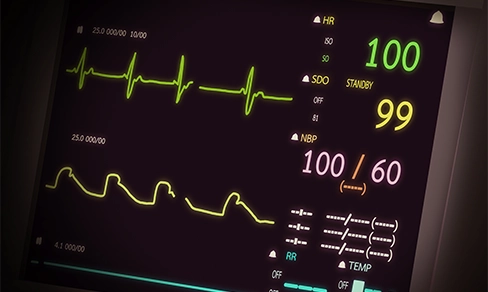
Although an EPS can be done under general anaesthetic, most are performed with a local anaesthetic. This means you will be awake during the procedure, and you may feel some pressure where the tubes are inserted, but you won’t feel any pain. We can also arrange for you to receive sedation during the EPS, if you feel this would be helpful. If we are using the electrical signals to produce extra beats in your heart, you may experience a racing sensation in your chest, or faintness / slight dizziness, but we can restore your heart to its natural rhythm within seconds if we need to. We will also be monitoring various vital signs during the test, such as your heartbeat, blood pressure and oxygen level.
How do I prepare for the procedure?
When you first come to see us, we’ll ask you about the medication you’re currently taking. It may be necessary to temporarily stop taking this medication in preparation for your Electrophysiology Study, but you should only do this in consultation with us – we will discuss this with you in detail before the test. On the day of the procedure, you’ll need to avoid eating and drinking for six hours beforehand. You will also need to arrange for someone to drive you to your appointment and collect you at the end.
What happens next?
Once the procedure has finished, we’ll take you back to the ward to rest – usually for one to two hours. The clinical team will monitor you and make sure you’re comfortable. We’ll then come and discuss the test results with you (if you were given a sedative, we’ll wait until the effects have worn off), and the next steps for your treatment. You will be given instructions about how and when to take any current or new medication. Most people are able to go home the same day as their EPS, though in some cases we may ask you stay overnight. Over the following day or two, you may feel some mild soreness where the catheter was inserted.
Patient’s thoughts

Jonathan’s Expertise
Common Questions
Book a Consultation
Reach out and book a consultation with Jonathan.
Expert TREATment
Heart Conditions
Experience expert treatment for heart conditions, with personalised care and advanced technology with Jonathan Lyne Heart Rhythm Cardiologist.
Extra heartbeats, usually harmless, occasionally need further investigation for caution.